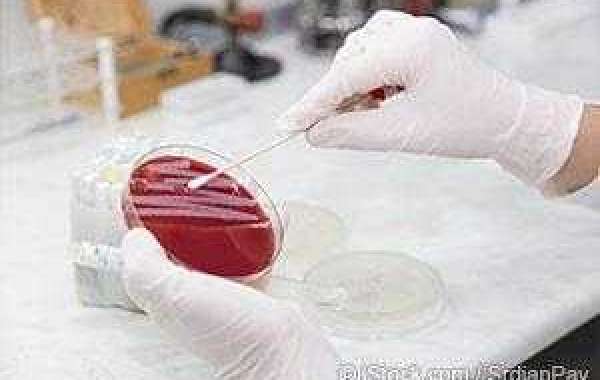
What does a staph infection look like? This type of infection is caused by the Staphylococcus aureus bacteria, and may come in two forms. The first is a skin infection, commonly marked by inflammation, the appearance of pus and rashes.
The second is an invasive infection, causing a myriad of symptoms such as a high fever, diarrhea and muscle pain.
Before Learning About Staph Infections, Learn About Staph Bacteria First
Staphylococcus is a type of bacteria that has 30 different species. When people use the term “staph infection,” they’re usually referring to the Staphylococcus aureus (S. aureus) subtype, which is the species responsible for most staph infections.
Around 15 to 40 percent of healthy people carry the S. aureus strain without developing diseases at all. The bacteria are typically found in your skin, nostrils or your flexures, which are the skin folds like your elbows, the back of your knees or underarms.1
Out in the open, staph bacteria can be anywhere, even in your food. This occurs when food isn’t properly handled, or when your kitchen or a restaurant has unsanitary conditions, allowing staph bacteria to grow on the food. Once ingested, it can lead to food poisoning.
Most times though, staph bacteria create diseases by entering through cracks in your skin or mucous membranes. Therefore, having healthy skin is important as it will serve as your first line of defense.
Finally, staph bacteria are incredibly resilient. Decades of using antibiotics to fight staph bacteria has caused staph bacteria to evolve and actually became immune to antibiotics, a condition known as methicillin-resistant Staphylococcus aureus (MRSA).
Although the name is taken from methicillin, an antibiotic originally used to treat staph infections, MRSA bacteria have actually become resistant to other antibiotics as well. The reason for their immunity is the presence of an extra gene that helps fight off penicillin-derived antibiotics whenever they are administered.2
How Staph Infections Are Diagnosed
Staph infections are often diagnosed in a clinical setting. A doctor may take a sample from your infection and create cultures to determine the microbe responsible for the infection. This is important because the diagnosis will depend on the type of bacteria you’re infected with.
If an experienced doctor is examining you, he might not need to collect a sample and can tell what kind of infection you have just by looking at it.3
People at Risk for Staph Infections
Staph bacteria can affect anyone at any age, but infants, toddlers and the elderly are more predisposed to these infections. This is most likely due to their weak immune systems that can’t fight off the sudden influx of bacteria in their system.
Those who are staying for an extended period of time in a hospital may develop a staph infection as well, a disease called HA-MRSA (hospital-acquired methicillin-resistant Staphylococcus aureus). It is very contagious and generally causes invasive infections. This happens when, for example, you’re recovering from a recent surgery and MRSA bacteria enters through the surgery incisions.
Among the general population, those who don’t wash their hands regularly may be at risk for a staph infection. They may develop one if they touch an infected surface and then rub their eyes afterward, causing pink eye. It’s possible for athletes to develop an infection as well if they come into direct contact with an infected person.